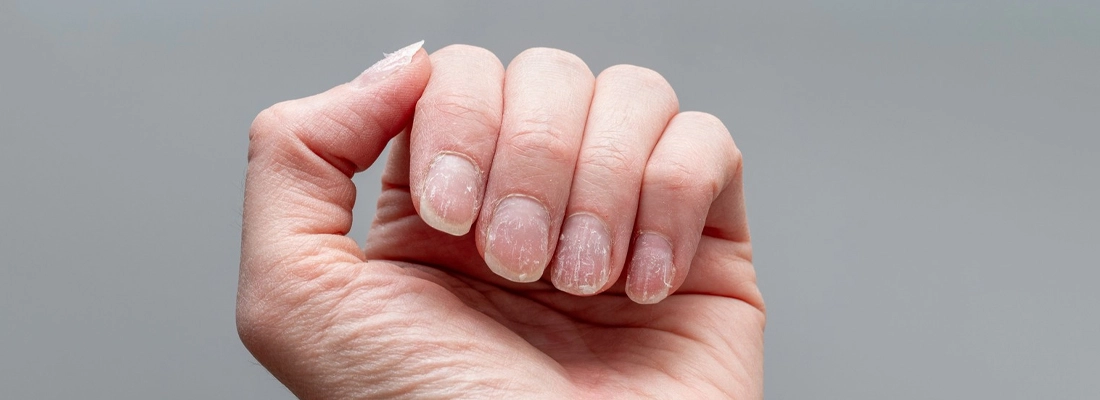
Did you know that the nails on your fingers and toes can tell stories about your health that your hair cannot? Just as a tree’s rings reveal its history, the subtle ridges, pits, or color changes in your nails may indicate deeper systemic changes. For people with alopecia areata, a condition primarily known for sudden hair loss, nails can serve as a silent companion in the disease’s journey, often overlooked but significantly informative.
While most discussions around alopecia areata focus on hair, nail changes are surprisingly common and can provide clues about disease severity, progression, and even prognosis. In fact, studies report nail involvement ranging from approximately 7% to 84% of patients with AA, with an average of about 22% experiencing noticeable changes. Nail changes are more frequent in severe forms of AA, such as AA totalis or AA universalis. These are reported more frequently in children and may be more common in males in some studies.
Understanding Nail Involvement in Alopecia Areata
The nails and hair share more than just visibility; both are formed by matrices of rapidly dividing cells susceptible to immune system attacks. In AA, cytotoxic T cells target the hair follicles, but they can also disrupt the proximal nail matrix. This leads to structural changes in the nails, often without causing pain, but sometimes creating cosmetic concerns or affecting quality of life.
Common signs of AA-related nail changes include:
- Pitting: Tiny, shallow depressions on the nail surface. Often described as small pinpoint depressions resembling marks made by a thumbtack; these pits are the most common nail change in AA.
- Trachyonychia (rough nails): Nails may become thin, brittle, or opaque with a sandpaper-like texture.
- Leukonychia: Small white spots or streaks on the nails, which can vary in size and number.
- Red lunula: A reddish discoloration of the half-moon area at the base of the nail.
- Longitudinal ridging: Vertical lines running along the length of the nail, giving it a textured appearance.
- Brittle or splitting nails: Nails may become fragile, breaking or splitting easily.
These alterations can appear before, during, or even after hair loss episodes. In some rare cases, nail changes are the first sign of AA, preceding any hair involvement. While typically asymptomatic, the visible changes can affect self-esteem and interfere with daily activities, especially for those who cannot cover them with nail polish.
What Causes Alopecia Areata Nails
The pathogenesis of alopecia areata nails involves immune system dysfunction. The immune system mistakenly attacks the nail matrix in a way similar to hair follicles, interrupting normal keratinization. Unlike hair follicles, nails do not scar from this inflammation, meaning that structural changes are usually reversible over time. However, the severity of inflammation correlates with the extent of nail involvement.
Factors that may influence alopecia areata nails include:
- Severity and duration of hair loss.
- Age of onset, with children often experiencing more pronounced nail changes.
- Genetic susceptibility and immune system factors.
- Overall health and presence of comorbid autoimmune conditions.
Because the appearance of alopecia areata fingernails can mirror disease severity, careful observation can help clinicians assess the broader impact of AA. Recognizing nail signs early can also guide treatment strategies and patient counseling.
When to Seek Diagnosis
Identifying nail changes associated with AA is generally clinical but may sometimes require additional testing. Dermatologists may perform:
- Visual examination: Evaluating nails for pitting, ridging, discoloration, and brittleness.
- Dermoscopy: Using a magnifying device to inspect fine surface changes.
- Biopsy: Rarely, when the diagnosis is uncertain or when nail dystrophy could be due to other causes.
Because nails grow slowly, changes may persist even after hair regrowth, and improvement is often gradual. In children, spontaneous resolution is more common, but adults may require treatment depending on cosmetic or functional concerns.
Also Read: How to Stop Alopecia Areata from Spreading
Treating and Managing Alopecia Areata Nails
Managing alopecia areata nails requires a thoughtful approach, balancing the severity of nail changes with cosmetic concerns and patient preferences. Unlike hair loss, nail involvement is often asymptomatic, and treatment is not always necessary. However, for those whose nails cause psychological stress or interfere with daily tasks, dermatologists may consider several interventions.
Treatment strategies include:
- Topical corticosteroids: Applied directly to the nails or surrounding cuticles, these can reduce inflammation and encourage normal nail growth.
- Intralesional corticosteroid injections: For more severe nail involvement, injections into the proximal nail fold may improve appearance and accelerate recovery.
- Topical minoxidil: Though primarily used for hair regrowth, minoxidil can sometimes support nail matrix activity.
- Systemic immunomodulators: In rare cases with extensive AA, medications that regulate the immune system may be prescribed.
- Supportive care: Keeping nails moisturized, trimming regularly, and avoiding trauma can prevent further cosmetic damage and improve nail strength.
It’s important to note that alopecia areata nails can improve spontaneously, especially in children, and aggressive treatments are often reserved for adults with severe or persistent changes. Patients should also be counseled on realistic expectations: nails grow slowly, so visible improvement may take months.
Before and After: What to Expect
Observing before and after alopecia nails can be reassuring for patients. In mild cases, pitting or ridging may fade as the nail grows out, while in severe cases, nail dystrophies may persist longer but gradually improve with consistent care. Monitoring nail growth over time also helps clinicians track disease activity and adjust treatment plans.
The Psychological Impact
Though nail changes are typically painless, their visible nature can affect self-esteem. People may feel self-conscious about showing their hands or feet, impacting social interactions or professional life. Addressing the psychological aspect is an important part of comprehensive care. Support groups, counseling, and patient education can help individuals cope with the visible effects of alopecia areata nails.
Diagnosing Nail Involvement Early
Early recognition of alopecia areata symptoms of nails can help differentiate them from other nail disorders, such as fungal infections, psoriasis, or trauma-related changes. Key indicators include:
- Sudden onset of nail pitting or ridging.
- Symmetrical involvement across multiple nails.
- Presence of concurrent hair loss or other autoimmune conditions.
A careful history and clinical examination usually suffice for diagnosis. In uncertain cases, dermoscopy or a nail matrix biopsy may provide definitive confirmation.
Causes and Risk Factors
Understanding the alopecia areata nails causes is essential for patient education and management. While the exact triggers are not fully understood, research suggests:
- Immune system dysregulation targeting the nail matrix.
- Genetic predisposition toward autoimmune responses.
- Association with severe or long-standing AA.
- Pediatric onset, which is often linked to more pronounced nail involvement.
By recognizing these factors, clinicians can anticipate potential nail changes and advise patients on monitoring and care.
Maintaining Healthy Nails During Alopecia Areata
Patients can take practical steps to support nail health:
- Keep nails clean, trimmed, and moisturized.
- Avoid harsh chemicals, acrylics, or trauma that could worsen dystrophy.
- Consider protective gloves during household chores.
- Regularly monitor nails for new changes to report to a dermatologist.
Conclusion
Nail involvement in alopecia areata is more than a cosmetic concern; it reflects the underlying immune activity of the disease. While alopecia areata nails are often asymptomatic, they can provide critical insights into disease severity and progression. Understanding the signs pitting, trachyonychia, leukonychia, red lunula, and brittle nails—helps patients and clinicians make informed decisions about care and management.
By recognizing, diagnosing, and managing alopecia areata fingernails early, patients can navigate the disease with confidence, understanding that improvement is often possible and that they are not alone in this journey. Ultimately, paying attention to the nails can provide a more complete picture of AA and guide better outcomes, both physically and emotionally.