What is a Maculopapular Rash?
A maculopapular rash is characterized by a combination of flat, discolored areas of the skin known as macules and small raised bumps called papules. These skin lesions typically manifest as red or pink and can cover a substantial area. In individuals with lighter skin, the rash may appear red, while in those with darker skin tones, it may manifest as a darker hue than the natural skin tone.
This type of rash is associated with various conditions, including childhood viruses like rubella and scarlet fever. However, it can also be attributed to allergic reactions, autoimmune diseases, HIV, or other underlying causes. The term “maculopapular” itself reflects its composition, with “macule” referring to flat discolored lesions and “papule” denoting small raised bumps. When macules exceed 1 centimeter, they are termed patches, and if papules merge, they form plaques.
Also read: Is Eczema An Autoimmune Disease?
Typically indicative of an infection, allergic reaction, or other underlying ailment, a maculopapular rash is considered a symptom rather than a standalone condition. It serves as a visual marker for a range of diseases, emphasizing the importance of consulting a doctor, especially when accompanied by other symptoms. Seeking medical attention is crucial as a maculopapular rash could signify a serious underlying illness, making a comprehensive evaluation essential for proper diagnosis and management.
Continue reading to learn more about what is a maculopapular rash. Its causes, appearance, and treatment options are available.
More Introduction:
Rashes can appear in a variety of ways, and discovering an unexplained patch of red, irritated skin can be distressing and uncomfortable. A maculopapular rash is a skin condition that is characterized by the presence of macules (flat discolored areas of skin) as well as papules (small, raised bumps) on the skin. This rash is marked by flat, discolored, and elevated lesions on the skin. It can be itchy and uncomfortable, and it may occur for a variety of reasons. Viral infections, allergic reactions, medication side effects, and certain systemic diseases can all cause maculopapular rashes
Treatment options include oral antihistamines, wet wraps, and topical creams. It is important to seek help from a healthcare professional for an accurate diagnosis and appropriate treatment.
Also read: A Comprehensive Guide to Living with Papular Eczema
Maculopapular Rash: Appearance
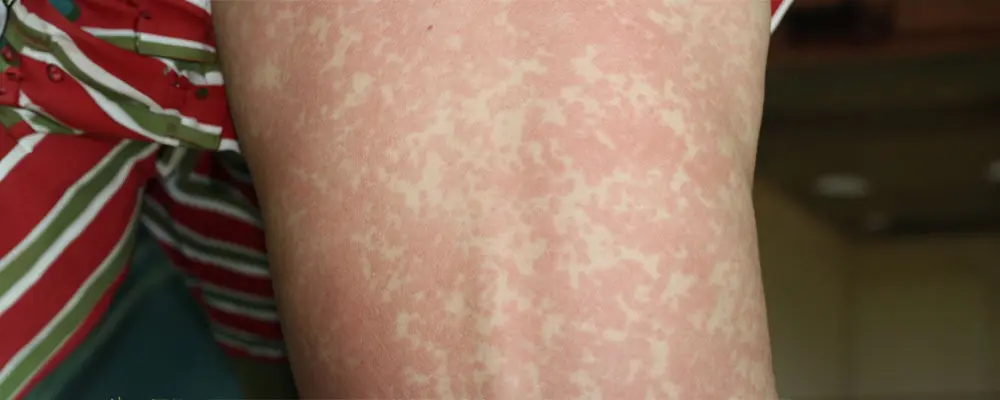
A maculopapular rash is often characterized by a combination of flat, discolored spots (macules) and small, raised bumps (papules) on the skin. Here are some key features of a maculopapular rash:
Macules:
Macules are flat and reddish or brownish in color. They are not raised or elevated above the skin’s surface. Macules are typically small, measuring a few millimeters to a centimeter in diameter. They can vary in shape and may merge to form larger patches.
Papules:
Papules are small, raised bumps that can be felt when running your fingers over the affected area. They are usually round or oval in shape and can be reddish or flesh-colored. Papules are typically less than a centimeter in diameter.
This rash can appear on the trunk, limbs, face, and extremities, among other areas of the body. The rash’s distribution may differ depending on the underlying cause. In some cases, the rash is generalized, affecting a large portion of the body, whereas, in others, it is localized to specific areas.
Rashes can cause itching or discomfort, depending on their severity. Itching can range from mild to severe, and scratching the rash can aggravate symptoms or lead to complications such as skin infections.
Maculopapular Rash & Atopic Dermatitis Resemblance:
A maculopapular rash and atopic dermatitis can have similar appearances. Both conditions can cause red, raised bumps on the skin, which can be confusing. It is important to note, however, that they have different underlying causes.
Atopic dermatitis, also known as eczema, is a chronic inflammatory skin condition characterized by an abnormal immune response and a weakened skin barrier. It is frequently associated with severe itching and a history of allergies. To have a better understanding, you can reach out to Clinical Research Organizations conducting Atopic Dermatitis Clinical Trials near you in Michigan.
Causes of Maculopapular Rash:
Several factors can cause a maculopapular rash, including:
- Viral infections: Many viral infections can cause a maculopapular rash. Examples include measles, rubella, roseola, chickenpox, and HIV/AIDS.
- Bacterial infections: Some bacterial infections can lead to a maculopapular rash, such as Lyme disease, syphilis, and meningococcemia.
- Allergic reactions: Allergies to certain foods, medications, or environmental triggers can result in a maculopapular rash. Common allergens include nuts, shellfish, penicillin, and latex.
- Drug reaction: Some medications can cause a maculopapular rash as a side effect. Antibiotics (e.g., penicillin, sulfonamides), anticonvulsants, nonsteroidal anti-inflammatory drugs (NSAIDs), and certain antiretroviral drugs used to treat HIV are known to trigger this type of rash.
- Autoimmune and systemic diseases: Certain autoimmune conditions and systemic diseases can manifest with a maculopapular rash. Examples include lupus, Kawasaki disease, vasculitis, and some types of drug reactions like Stevens-Johnson syndrome.
- Insect bites: Bites from certain insects, such as fleas, mites, or bedbugs, can cause a maculopapular rash in some individuals.
- Environmental factors: Exposure to certain chemicals, plants, or environmental factors can lead to a maculopapular rash. For instance, contact dermatitis is caused by coming into contact with irritants like poison ivy or certain chemicals.
Also read: What Causes Eczema Flare-ups?
Maculopapular Rash: Diagnosis:
A doctor will ask about a person’s general health as well as any history of illness or allergies to determine the cause of this rash. They will inquire as to where and when the rash appeared on the body.
A doctor will also inquire about:
- Any medications that the individual is taking in the presence of other symptoms.
- Travel history especially to areas where viral infections are prevalent.
- A physical examination will then be performed by the doctor. To check for infection, they may order blood or urine tests. They may take a small sample of the rash (a biopsy) to look at under a microscope.
Treatment of Maculopapular Rash:
It is essential to identify and address the specific cause to effectively manage the rash. Treatment for this condition includes both symptom relief and addressing the underlying cause. If there is a risk of anaphylaxis, you will be given epinephrine right away.
- Treating underlying infection: For a rash caused by infection, timely treatment with prescribed antiviral or antibiotic medication is vital. Completing the full course of medication is crucial for effective treatment.
- Allergy management: identifying and avoiding allergens for allergy-related rashes is key. Antihistamines can be prescribed to alleviate itching. In severe cases, immediate medical attention and possibly an EpiPen may be necessary.
- Medication modifications: If a rash is a known medication side effect, consult a healthcare professional before making any changes. They may adjust dosage or switch medications as needed.
- Symptomatic relief: Topical treatments such as corticosteroid creams or ointments may be prescribed to relieve symptoms such as itching and inflammation. These can help with itching, redness, and inflammation caused by the rash.
The goals of maculopapular rash treatment are to address the underlying cause, reduce symptoms, and get rid of the rash as early as possible.
Also read: Popular Urticaria – A Comprehensive Guide and Is It Contagious?
Home Remedies for Maculopapular Rashes:
For treatment of rashes at home, consider these remedies:
- Apply wet compresses: Apply cool or wet compresses by placing a damp cloth on the rash for 15 to 30 minutes multiple times a day.
- Bath: Take cool baths and add baking soda or oatmeal bath products to ease itching.
- Avoid scratching: Avoid scratching to prevent infections; consider using a gauze dressing to cover the rash.
- Go easy on yourself: Skip soap if needed, wash with cool water, and pat rashes dry instead of rubbing.
Use anti-itch cream: Use anti-itch creams for minor allergic rashes.
If home remedies do not work, it’s advisable to seek guidance from your doctor.
Takeaway:
A maculopapular rash is characterized by the presence of both a flat, discolored area of skin (macule) and raised bumps (papules). The rash can be caused by a number of infections, medical conditions, or substance exposures. Some rashes resolve on their own, while others may require treatment. Depending on the cause, treatment may include treating infections with antiviral or antibiotic medications, managing allergies with avoidance and antihistamines, adjusting or discontinuing triggering medications, and providing symptomatic relief with topical corticosteroids. It is best to consult with an experienced healthcare professional who can assist you in managing the condition better.




