Introduction
Prurigo Nodularis (PN) is a chronic skin condition characterized by itchy, raised, and frequently excoriated (scratched) nodules on the skin. These nodules are typically firm and dome-shaped, with diameters ranging from a few millimeters to several centimeters as you will check prurigo nodularis pictures below in this article. Scratching can aggravate the rash and lead to secondary infections. Relief from itching is part of the treatment.
It can appear anywhere on the body, but it is most common in a symmetrical pattern on the arms, legs, back, and torso. Because it is the most severe form of prurigo, it can be difficult to treat. The itching associated with PN can be severe and persistent, affecting the individual’s quality of life significantly.
Continue reading to know what is prurigo nodularis? What does it look like? What causes prurigo nodularis, its triggers, and the best treatment options available.
Also, read: Foods to Avoid if you have Prurigo Nodularis
What is Prurigo Nodularis?
Prurigo nodularis is a chronic skin condition that can develop on its own or in conjunction with another medical condition. The nodules that form are so itchy that people with prurigo nodularis frequently encounter other problems, such as sleep disturbances and psychological distress.
Extreme itching can also cause people to scratch an area until it bleeds or becomes painful. Itchy skin can be caused by a variety of factors, including:
• Scaly skin
• Thyroid disorder
• Chronic kidney disease
The itching caused by PN can be incapacitating. It is thought to have the most intense itch of any itchy skin condition. Scratching aggravates the itching and can result in the formation of new bumps as well as the worsening of existing bumps.
What Causes Prurigo Nodularis?
The exact cause of Prurigo Nodularis is unknown, but it is thought to be a complex and multifactorial disorder. What triggers prurigo nodularis is mentioned below:
Skin Irritation and Scratching:
Constant scratching or rubbing of the skin, often as a result of an initial itch caused by another skin condition, insect bites, or irritation, can result in the formation of nodules. Scratching can cause a cycle of itching and scratching, resulting in the formation of nodules.
Neurogenic Factors:
Prurigo nodularis is thought to be caused by nerve and nerve-ending abnormalities in the skin. These abnormalities can cause increased itching sensitivity and an exaggerated reaction to minor irritants.
Neurotransmitters:
These are chemicals that allow nerve cells to communicate with one another. Neurotransmitter imbalances, such as substance P and histamine, can contribute to the intense itching experienced by people with PN.
Inflammatory Factors:
There is evidence that inflammation may play a role in the progression of prurigo nodularis. The itch-scratch cycle and the formation of nodules can be aided by inflammatory cells and molecules in the skin.
Underlying Skin Conditions:
Skin conditions such as eczema, atopic dermatitis, and chronic pruritus (itching) are frequently associated with nodularis. These conditions can set off the itch-scratch cycle, which leads to the formation of nodules.
Psychological Factors:
Emotional stress, anxiety, and psychological factors can exacerbate itching and scratching behaviors, potentially contributing to prurigo nodularis persistence.
Genetics:
While not fully understood, there may be a genetic predisposition that increases the likelihood of developing PN in certain people.
What does PN look like? Prurigo Nodularis Pictures
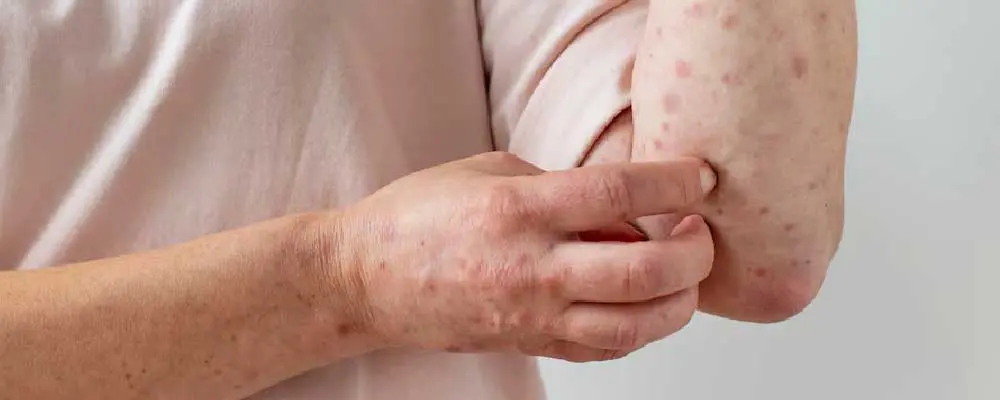
Prurigo nodularis pictures show the nodules appearing as clusters of raised, firm nodules on the skin’s surface. These nodules, which range in size from a few millimeters to several centimeters, are colored from red to brown or skin-colored. The surface may be scaly or rough, with signs of scratching such as erosions or crusts.
Commonly found on the extensor surfaces of the arms and legs, occasionally extending to the trunk, the condition can manifest with a few lesions or numerous ones, sometimes numbering in the hundreds. Prurigo nodularis pictures are shared for the reference with their types explained below:
1- Prurigo Nodularis Type 1: Classic Prurigo Nodularis
Multiple itchy nodules ranging in color from pink to brown are frequently present. They can be extremely itchy and become excoriated as a result of scratching. See Prurigo nodularis pictures here.
2- Prurigo Nodularis Type 2: Hypertrophic Prurigo Nodularis
The nodules are particularly thickened and may have a more pronounced “lichenified” appearance. Lichenification is the thickening and hardening of the skin caused by repeated rubbing or scratching.
3- Prurigo Nodularis Type 3: Early Lesional Prurigo Nodularis
This subtype describes newly formed nodules. Before they fully develop into the characteristic nodules seen in PN, they may appear as small, erythematous papules.
4- Prurigo Nodularis Type 4: Excoriated Prurigo Nodularis
This type is distinguished by scratched nodules that result in open sores, scabs, and crusted lesions. Excoriated PN can be caused by the obsessive scratching associated with intense itchiness. See Excoriated Prurigo Nodularis Pictures.
Is Prurigo Nodularis Life-threatening?
A common question most often arises, can prurigo nodularis kill you?
While prurigo nodularis is not considered a life-threatening condition, the persistent itching and discomfort it causes can have a significant impact on a person’s quality of life. Prolonged scratching can cause skin breaks, increasing the risk of infection. As a result of the constant scratching and inflammation associated with prurigo nodularis, bacterial infections or other skin complications can occur in some cases.
Itching caused by PN can be extremely distressing, causing sleep disturbances, anxiety, and depression. This repeated scratching not only stresses the severe pruritus that comes along with the condition, but it also helps form secondary changes like abrasion, further complicating the clinical presentation.
What is the Best Treatment for Prurigo Nodularis?
It can be difficult to treat prurigo nodularis, and the best approach varies from person to person. It is important to seek personalized advice from a dermatologist or medical professional.
Among the possible treatments for prurigo nodularis are:
• Topical Corticosteroids: In mild to moderate cases, topical corticosteroids can help reduce inflammation and itching.
• Calcineurin Inhibitors (Topical): These are non-steroidal creams that can help with inflammation and itching. Tacrolimus and pimecrolimus are two examples.
• Antihistamines: If itching is a significant symptom, antihistamines taken orally can help relieve itching and improve sleep quality.
• Topical Capsaicin: This is a chili pepper cream that can help relieve itching by desensitizing nerve fibers.
• Phototherapy: Light therapy, such as ultraviolet B (UVB) or ultraviolet A (UVA) can be helpful in the treatment of prurigo nodularis.
• Systemic Therapies: Oral medications such as corticosteroids, cyclosporine, methotrexate, or other immune-modulating drugs may be considered in more severe cases.
• Gabapentin or Pregabalin: These medications can help relieve itching and discomfort caused by nerves.
• Psychological Support: Because prurigo nodularis can be exacerbated by stress and anxiety, therapy or counseling may help manage symptoms.
• Immunosuppressants: In severe cases, immunosuppressive medications such as azathioprine or mycophenolate mofetil may be considered.
It is essential to work closely with a dermatologist to determine the best treatment plan based on one’s severity of the condition.
Outlook
Prurigo nodularis is a chronic, inflammatory skin condition. The itch will be the first thing to be noticed, but the more the sufferer will scratch, the more damage it will cause to the skin. After a while, bumps or nodules form. The spots start small but can grow to be as large as a quarter. Scratching may also cause burning, bleeding, and lesions in the affected area. Although there is no known cause of prurigo nodularis, most cases are caused by an underlying health disorder.
Along with a physical examination, the doctor will perform a skin biopsy or dermoscopy to rule out other skin disorders. Numerous clinical research organizations working on finding better treatment options, but diagnosing prurigo nodularis and any potential co-occurring conditions must come first.




